Many adults assume wisdom tooth pain strikes suddenly, but impacted wisdom teeth often develop gradually, causing discomfort that builds over months or years. Understanding the symptoms, classifications, and treatment criteria for impacted wisdom teeth empowers you to make informed decisions about your oral health and when extraction becomes necessary.
Table of Contents
Toggle- Table of Contents
- Key takeaways
- What are impacted wisdom teeth?
- Symptoms and diagnosis of impacted wisdom teeth
- Classification and risks of impacted wisdom teeth
- Do impacted wisdom teeth need to come out? criteria for extraction
- What to expect from wisdom tooth removal and recovery
- Discover expert wisdom tooth care at Bespoke Dental Fulham
- Frequently asked questions about impacted wisdom teeth
- Recommended
Table of Contents
- What Are Impacted Wisdom Teeth?
- Symptoms And Diagnosis Of Impacted Wisdom Teeth
- Classification And Risks Of Impacted Wisdom Teeth
- Do Impacted Wisdom Teeth Need To Come Out? Criteria For Extraction
- What To Expect From Wisdom Tooth Removal And Recovery
- Discover Expert Wisdom Tooth Care At Bespoke Dental Fulham
- Frequently Asked Questions About Impacted Wisdom Teeth
Key takeaways
| Point | Details |
|---|---|
| Common timing | Impacted wisdom teeth typically cause problems between ages 17 and 25, though symptoms can appear later. |
| Diagnostic necessity | X-rays are essential for detecting impaction, as visual examination alone cannot reveal tooth position beneath gums. |
| Warning signs | Symptoms include jaw pain, gum swelling, bad breath, and difficulty chewing, often developing gradually rather than suddenly. |
| Potential complications | Untreated impaction can lead to infections, damage to adjacent teeth, gum disease, and in rare cases cysts. |
| Individual assessment | Not all impacted wisdom teeth require removal; decisions depend on clinical evaluation of symptoms and risks. |
What are impacted wisdom teeth?
Impacted wisdom teeth are third molars that fail to emerge properly through the gums due to insufficient space in the jaw or misalignment during development. These teeth become trapped, either partially or completely, beneath the gum tissue or within the jawbone.
Wisdom teeth typically erupt between ages 17 and 25, though not everyone develops them. Modern diets require less grinding force than ancestral diets, making wisdom teeth largely vestigial structures with minimal functional value. When space limitations prevent proper eruption, these teeth can develop at various angles, creating complications that affect surrounding structures.
Impacted wisdom teeth represent one of the most common dental issues among young adults. The position and degree of impaction vary considerably between individuals, influencing both symptoms and treatment approaches. Understanding whether your wisdom teeth are impacted requires professional assessment, as many cases develop without obvious external signs.
Several symptoms may indicate wisdom tooth impaction:
- Persistent or recurring jaw pain
- Swollen, tender, or bleeding gums around the back molars
- Difficulty opening your mouth fully
- Unpleasant taste or bad breath that persists despite hygiene
- Headaches or referred pain to the ear or neck
If you experience recurring discomfort in the back of your mouth, consulting your dentist promptly helps determine whether wisdom tooth removal is necessary before complications develop.
Symptoms and diagnosis of impacted wisdom teeth
Recognising impacted wisdom teeth symptoms early prevents more serious complications. Unlike the sudden sharp pain many expect, discomfort from impaction typically begins as a low-level ache or gum irritation that gradually intensifies.
Common symptoms include pain, swollen and bleeding gums, swelling around the jaw, bad breath, headache or jaw ache, and an unpleasant taste when eating. These signs often appear intermittently rather than continuously, with flare-ups occurring during periods of stress or illness when immunity decreases. Some patients notice difficulty chewing on the affected side or feel a constant pressure sensation behind their second molars.

Recurring pain suggests ongoing problems that require professional evaluation. Pain patterns vary, some patients experience sharp, localised discomfort whilst others describe a dull, radiating ache extending into the jaw, ear, or temple. Swelling may cause visible facial asymmetry during acute episodes.
Diagnosing impacted wisdom teeth relies heavily on imaging technology. The only reliable way to know whether you have wisdom teeth and whether they are impacted is with a dental X-ray. Panoramic X-rays, also called OPG X-rays, provide comprehensive views of all four wisdom teeth simultaneously, revealing their positions, angles, and relationship to adjacent structures including nerves and sinuses.
Pro tip: Schedule regular dental check-ups with X-rays every 18 to 24 months during your late teens and twenties to identify impactions before symptoms emerge, allowing for proactive treatment planning.
Early detection through routine imaging often reveals impactions in asymptomatic patients, enabling dentists to monitor development and intervene strategically. When symptoms do appear, prompt consultation prevents progression to infections or damage. Sedation options are available for anxious patients requiring treatment, and emergency dental services address acute pain episodes.
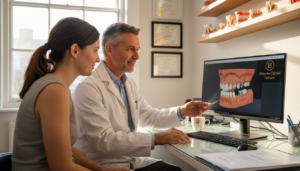
Classification and risks of impacted wisdom teeth
Impacted wisdom teeth are classified based on their position within the jaw and the degree of eruption. Understanding these classifications helps clarify your specific condition and associated risks.
Three main classification types exist: soft tissue impaction, partial bony impaction, and complete bony impaction. Soft tissue impaction occurs when the tooth has penetrated through the bone but remains covered by gum tissue. Partial bony impaction means the tooth is partially erupted but remains partly embedded in the jawbone. Complete bony impaction describes teeth fully encased within the jaw with no eruption through bone or gum.
Additionally, impactions are categorised by angular orientation:
- Vertical impaction: tooth positioned upright but blocked from erupting
- Mesial impaction: tooth angled forward toward the front of the mouth
- Horizontal impaction: tooth lying sideways within the jaw
- Distal impaction: tooth angled backward toward the throat
Horizontal and mesial impactions commonly cause damage to adjacent molars, as the impacted tooth presses against the roots or crown of the second molar. This pressure can lead to root resorption, decay, or structural compromise of otherwise healthy teeth.
| Impaction type | Characteristics | Typical risks |
|---|---|---|
| Soft tissue | Crown emerged through bone, covered by gum | Infection, pericoronitis, decay |
| Partial bony | Partly through bone, partly buried | Bone loss, cyst formation, adjacent tooth damage |
| Complete bony | Fully encased in jawbone | Cyst development, nerve proximity concerns |
| Horizontal | Tooth lying sideways | Severe damage to second molar, bone complications |
| Mesial | Angled toward front teeth | Crowding, root damage to adjacent teeth |
Untreated impacted wisdom teeth can lead to gum disease, tooth decay, damage to other teeth, and in rare cases cysts and tumours. Partially erupted teeth create pockets where bacteria accumulate, causing recurring infections called pericoronitis. These infections produce pain, swelling, difficulty swallowing, and fever in severe cases.
Pro tip: If extraction is not immediately recommended, maintain meticulous oral hygiene around wisdom teeth and attend regular monitoring appointments to detect changes early.
Cysts can develop around impacted wisdom teeth, gradually expanding and damaging surrounding bone and tooth roots. Whilst rare, these complications underscore the importance of professional monitoring. Understanding your impaction type and associated risks helps you participate actively in treatment decisions, whether that involves extraction or continued observation. For patients concerned about other teeth, dental implants can replace damaged molars, whilst gum disease treatment addresses inflammation caused by impaction.
Do impacted wisdom teeth need to come out? criteria for extraction
Not all impacted wisdom teeth require removal. Extraction decisions should be made case by case, considering overall oral health, tooth position, and potential for future problems. Dentists evaluate multiple factors through clinical examination and radiographic analysis before recommending treatment.
Key criteria prompting extraction include:
- Recurring pain or discomfort that affects daily activities
- Repeated infections or pericoronitis episodes
- Damage to adjacent teeth, including decay or root resorption
- Cyst formation or bone loss around the impacted tooth
- Orthodontic concerns where wisdom teeth compromise alignment
- Inability to clean the area properly, leading to chronic inflammation
Dentists assess impaction severity, angulation, proximity to nerves, and your age when formulating recommendations. Younger patients typically experience easier extractions and faster healing, as roots are less developed and bone is less dense. However, age alone does not dictate treatment, asymptomatic impactions in older adults may be safely monitored indefinitely.
Some impacted wisdom teeth remain completely asymptomatic throughout life and never require intervention. Regular monitoring through periodic X-rays and examinations ensures changes are detected promptly. Your dentist will discuss risk versus benefit, considering factors including surgical complexity, healing expectations, and long term oral health goals.
Surgical extraction is common treatment for symptomatic impacted wisdom teeth. The procedure involves accessing the tooth through gum tissue and sometimes bone, then sectioning the tooth for removal. Complexity varies based on impaction depth and angle.
Seek professional evaluation if you experience persistent symptoms or if routine X-rays reveal developing impactions. Understanding when wisdom tooth removal becomes necessary helps you plan appropriately. A comprehensive wisdom tooth removal guide can clarify the process and set realistic expectations.
What to expect from wisdom tooth removal and recovery
Understanding the extraction procedure and recovery timeline helps you prepare mentally and practically for wisdom tooth removal.
Surgical extraction is the standard approach for impacted wisdom teeth. The procedure begins with anaesthesia, ranging from local numbing to sedation or general anaesthesia depending on case complexity and patient preference. Your oral surgeon makes an incision in the gum tissue, removes any obstructing bone, and extracts the tooth, sometimes sectioning it into smaller pieces for easier removal. The site is then cleaned and sutured.
Recovery typically ranges from 7 to 14 days. Most patients experience peak swelling and discomfort during the first 48 to 72 hours, gradually improving thereafter. Normal healing signs include:
- Mild to moderate swelling that peaks on day two or three
- Bruising around the jaw and cheeks
- Stiffness when opening your mouth
- Minor bleeding or oozing for the first 24 hours
- Temporary numbness if nerves were near the extraction site
Pain management combines prescribed or over-the-counter medications with cold compresses during the first few days. Most patients return to normal activities within a week, though complete bone healing requires several months. Soft foods, gentle rinsing with salt water, and avoiding straws or smoking promote optimal healing.
Pro tip: Follow all post-operative care instructions meticulously, including dietary restrictions and hygiene protocols, to minimise complications like dry socket or infection.
Potential complications include dry socket, where the blood clot dislodges prematurely, causing severe pain and delayed healing. Infection, prolonged numbness, or sinus complications occur rarely but require prompt dental attention. Contact your dentist immediately if you experience increasing pain after day three, high fever, difficulty breathing or swallowing, or excessive bleeding.
Sedation options ranging from oral sedatives to IV sedation ensure comfort throughout the procedure. Discussing your anxiety levels and medical history with your oral surgeon helps determine the most appropriate approach. Understanding the wisdom tooth extraction process reduces uncertainty and builds confidence in your treatment plan.
Discover expert wisdom tooth care at Bespoke Dental Fulham
If you are experiencing symptoms of impacted wisdom teeth or seeking professional evaluation, Bespoke Dental Fulham offers expert assessment and treatment tailored to your unique oral health needs. Our experienced team utilises advanced digital imaging to accurately diagnose impaction and develop personalised treatment plans that prioritise your comfort and long term dental wellness.
Whether you require extraction or monitoring, we provide comprehensive care in a discreet, serene environment designed for your comfort. Beyond wisdom tooth management, our cosmetic dentistry services including veneers, whitening, and orthodontics help you maintain a confident smile throughout your dental journey. Our wisdom tooth extraction services combine surgical precision with patient-centred care, whilst our dental hygiene therapy supports optimal oral health during recovery. Schedule a consultation today to gain clarity and peace of mind about your wisdom teeth.
Frequently asked questions about impacted wisdom teeth
Do all impacted wisdom teeth need to be removed?
No, not all impacted wisdom teeth require extraction. Asymptomatic teeth that cause no pain, infection, or damage to adjacent structures can often be monitored indefinitely through regular dental examinations and X-rays. Removal becomes necessary only when complications arise or risks outweigh benefits of retention.
What happens if I ignore my impacted wisdom teeth?
Ignoring symptomatic impacted wisdom teeth can lead to serious complications including chronic infections, damage to neighbouring teeth, bone loss, cyst formation, and severe pain. Early intervention prevents these issues and typically results in simpler procedures with faster recovery compared to treating advanced complications.
How do I know if my wisdom teeth are causing problems?
Common indicators include persistent jaw pain, swollen or bleeding gums around back molars, bad breath despite good hygiene, difficulty opening your mouth, and recurring infections. However, many impactions develop without symptoms, making regular dental X-rays essential for detection.
What pain management options are available before extraction?
Before extraction, over-the-counter pain relievers, salt water rinses, and cold compresses can temporarily manage discomfort. Your dentist may prescribe antibiotics for active infections and stronger pain medication for severe episodes, though these provide only temporary relief until definitive treatment occurs.
Can impacted wisdom teeth affect my smile or facial appearance?
Impacted wisdom teeth rarely affect facial appearance directly, though severe infections can cause temporary facial swelling. Complications like damage to adjacent teeth or bone loss may indirectly impact your smile’s aesthetics and function, making timely treatment important for maintaining oral health and appearance.