Wisdom teeth, or third molars, are the last teeth to emerge, typically appearing in your late teens or early twenties. Many people assume that if they’re not causing pain, there’s no reason to act. But that belief can lead to serious consequences. Silent problems, from infection to cyst formation and decay on neighbouring teeth, can develop over months or even years before you notice anything wrong. Understanding why removing problematic wisdom teeth matters, and when to act, puts you in control of your long-term oral health rather than waiting for a crisis to force your hand.
Table of Contents
Toggle- Table of Contents
- Key Takeaways
- How wisdom teeth cause hidden dental problems
- When extraction makes sense: evidence and expert perspectives
- Who benefits most from wisdom tooth extraction?
- Caring for your mouth after extraction: preventing further issues
- Why proactive care matters more than one-size-fits-all removal
- Considering extraction? Fulham’s experts can help
- Frequently asked questions
- Recommended
Table of Contents
- How wisdom teeth cause hidden dental problems
- When extraction makes sense: evidence and expert perspectives
- Who benefits most from wisdom tooth extraction?
- Caring for your mouth after extraction: preventing further issues
- Why proactive care matters more than one-size-fits-all removal
- Considering extraction? Fulham’s experts can help
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Impacted teeth cause problems | Wisdom teeth that don’t erupt properly can silently lead to bigger dental issues. |
| Extraction isn’t always required | Routine removal isn’t necessary for healthy, symptom-free wisdom teeth—monitoring is often safer. |
| Personal risk matters | Older adults, smokers, and those with impaction or decay benefit most from timely extraction. |
| Aftercare aids healing | Following recovery advice prevents complications and supports a smooth healing process. |
How wisdom teeth cause hidden dental problems
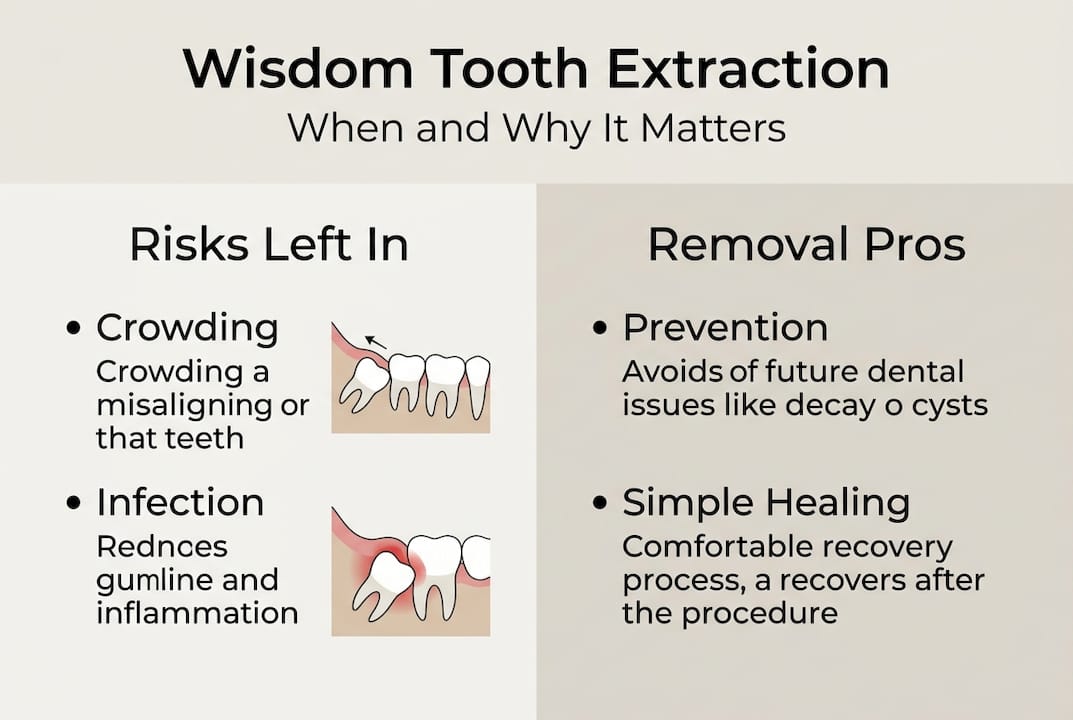
Wisdom teeth often cause trouble not because they’re inherently problematic, but because the modern jaw simply doesn’t have enough room for them. When there isn’t sufficient space, these teeth become impacted, meaning they’re unable to fully erupt through the gum. Some tilt sideways, pressing against the tooth in front. Others partially break through the gum, leaving a flap of tissue that traps bacteria. Many stay buried entirely beneath the bone.
The difficulty is that none of these scenarios necessarily cause pain straight away. You might feel fine for years while damage quietly accumulates. Impacted wisdom teeth are notoriously hard to clean, and the Cleveland Clinic confirms that impacted teeth cause decay and gum disease in adults when left in place. The toothbrush simply cannot reach these areas effectively.
Here are the most common complications that develop when problematic wisdom teeth are left untreated:
- Pericoronitis: Infection of the gum tissue surrounding a partially erupted tooth, causing swelling, pain, and sometimes fever
- Decay on adjacent teeth: The second molar sits directly in front of the wisdom tooth and is particularly vulnerable to cavities caused by trapped food and bacteria
- Cyst formation: Fluid-filled sacs can develop around impacted teeth, damaging bone and nearby tooth roots over time
- Gum disease: Chronic inflammation around wisdom teeth can spread, affecting the health of surrounding teeth and supporting bone
- Crowding: Pressure from emerging wisdom teeth may contribute to shifting of the front teeth, though evidence on this is mixed
“The real risk isn’t always dramatic. It’s the slow, invisible damage to adjacent teeth and bone that catches patients off guard.”
Knowing whether you should extract wisdom teeth early is far better than waiting until a cyst has eroded bone or decay has spread to a healthy molar. The cost, both financially and in terms of treatment complexity, rises considerably once complications take hold.
When extraction makes sense: evidence and expert perspectives
The decision to extract isn’t always straightforward. Evidence and clinical opinion vary, and that’s worth acknowledging honestly.
A Cochrane review found that for asymptomatic, disease-free teeth, there is insufficient evidence to recommend routine prophylactic removal, suggesting monitoring as the preferred approach. However, as noted in a review of contrasting clinical views, institutions such as the Cleveland Clinic advocate for preventive removal to avoid future complications, particularly in younger patients.
This isn’t a contradiction. It reflects the reality that each patient’s situation is different.
| Scenario | Recommended approach |
|---|---|
| Fully erupted, healthy, cleanable | Monitor with regular X-rays |
| Partially erupted with recurring infection | Consider extraction |
| Impacted with adjacent tooth decay | Extraction strongly advised |
| Asymptomatic but high-risk patient profile | Discuss with your dentist |
| Cyst or bone loss present | Extraction recommended |
The pros and cons of extraction depend heavily on your age, the position of the tooth, and your overall oral health. Younger patients tend to recover faster and face fewer surgical risks. Bone is softer, roots are less developed, and healing is quicker.
Pro Tip: If your dentist recommends monitoring your wisdom teeth, ask specifically what signs or changes would trigger a recommendation for extraction. Having a clear threshold helps you stay informed rather than anxious.
For a thorough overview of what the process involves, the Fulham wisdom tooth extraction guide covers the procedure, costs, and what to expect from start to finish.
Who benefits most from wisdom tooth extraction?
Not everyone needs their wisdom teeth removed. But certain profiles carry a much higher risk of complications, and for these patients, proactive extraction makes strong clinical sense.
Research published in 2025 identified key risk factors for post-operative complications including older age, smoking, low BMI, and complex impaction patterns. Conversely, surgical technique, specifically the use of a trapezoidal flap, was found to be protective. This tells us that both patient factors and clinical skill matter significantly.
Here’s a numbered breakdown of who should most seriously consider extraction:
- Patients with recurring pericoronitis: If you’ve had two or more episodes of infection around a wisdom tooth, the pattern is unlikely to stop without removal
- Those with adjacent molar decay: When the second molar is already being affected, continuing to wait increases the risk of losing a tooth that would otherwise be healthy for decades
- Younger adults aged 18 to 25: Recovery is faster, roots are shorter, and the risk of nerve involvement is generally lower
- Patients with cysts or bone changes: Detected on X-ray, these require prompt attention regardless of symptoms
- Smokers or those with compromised immune systems: Higher infection risk makes monitoring alone less reliable
| Patient factor | Risk level | Suggested action |
|---|---|---|
| Age 18 to 25, impacted | Moderate | Discuss extraction timing |
| Recurring infection | High | Extraction advised |
| Adjacent tooth decay | High | Extraction recommended |
| Asymptomatic, healthy | Low | Monitor with X-rays |
| Smoker with impaction | High | Early extraction advised |
Pro Tip: Ask your dentist to show you your panoramic X-ray and explain the exact position of each wisdom tooth. Seeing the angle and depth yourself makes the decision far less abstract.
If you’ve decided to proceed, preparing for extraction well in advance, including arranging time off and understanding what to eat beforehand, makes a real difference to your experience. For those considering private care, the private oral surgery guide outlines what to expect from a premium clinical setting.
Caring for your mouth after extraction: preventing further issues
Preventing greater dental problems does not stop at extraction. Careful aftercare is just as critical to a successful outcome.

The first 24 to 48 hours are the most important. A blood clot forms in the socket and acts as the foundation for healing. Disturbing this clot, whether through rinsing too vigorously, drinking through a straw, or smoking, can lead to dry socket, a painful condition that delays recovery significantly.
The wisdom tooth recovery guide provides a day-by-day breakdown of what to expect, while post-removal recovery tips offer practical advice for managing swelling, diet, and activity levels.
Key aftercare steps to follow:
- Bite gently on gauze for the first hour to control bleeding and support clot formation
- Avoid rinsing or spitting for the first 24 hours to protect the socket
- Eat soft foods such as yoghurt, soup, and mashed potato for the first few days
- Keep the area clean by gently rinsing with warm salt water from day two onwards
- Avoid smoking and alcohol for at least 72 hours, as both impair healing and raise infection risk
- Take prescribed pain relief as directed, rather than waiting until discomfort becomes severe
Most people feel significantly better within five to seven days. Complex extractions or those involving impacted teeth may take a little longer. If you experience worsening pain after the third day, a foul taste, or visible bone in the socket, seek advice promptly. Guidance on preventing dry socket and understanding pain after extractions can help you distinguish normal healing from something that needs attention.
Good hygiene habits and attending your follow-up appointments are the final pieces of the puzzle. The same evidence that highlights the risks of leaving impacted teeth in place also underscores how much ongoing oral hygiene and professional review matter to long-term outcomes.
Why proactive care matters more than one-size-fits-all removal
At Bespoke Dental Fulham, we see a consistent pattern: patients who delay acting on wisdom teeth often do so because nothing hurts. By the time pain arrives, the situation is frequently more complex than it needed to be.
The evidence does not support removing every wisdom tooth as a matter of routine. But it strongly supports regular monitoring, honest clinical assessment, and timely extraction when the signs are there. The mistake isn’t removing wisdom teeth. It’s assuming that the absence of pain means the absence of a problem.
We also notice that patients often feel reassured, not alarmed, once they understand what’s actually happening in their mouth. Seeing your own X-ray, understanding the position of each tooth, and having a clear plan removes uncertainty. That’s what individualised extraction advice looks like in practice. It’s not about pushing treatment. It’s about giving you the information to make a confident, informed decision.
Considering extraction? Fulham’s experts can help
If this article has raised questions about your own wisdom teeth, the most useful next step is a proper assessment. Not a general opinion, but a clinical review with X-rays and a clear conversation about your specific situation.
At Bespoke Dental Fulham, we offer personalised consultations that look at your full oral health picture, not just the tooth causing concern. Whether you’re weighing up the pros and cons of wisdom tooth removal or simply want to understand your options, our team is here to guide you. Explore our general dental services or visit our Fulham dental practice to book a consultation and take the first step towards clarity.
Frequently asked questions
What are the main risks of not removing wisdom teeth?
Retained wisdom teeth can lead to decay, infection, and gum disease even without any initial pain, particularly when they’re impacted and difficult to clean properly.
Do all wisdom teeth need to be extracted?
No. Asymptomatic, disease-free wisdom teeth are generally monitored rather than routinely removed, with extraction recommended only when symptoms or clinical risk factors emerge.
Who should consider wisdom tooth extraction most seriously?
Patients with recurring infections, adjacent tooth decay, or risk factors such as older age and smoking should discuss extraction with their dentist sooner rather than later.
How long is recovery after wisdom tooth extraction?
Most people feel significantly better within five to seven days, though complex or deeply impacted cases may require a longer healing period.
How can I prevent complications after removal?
Follow your dentist’s aftercare instructions carefully, avoid smoking and alcohol in the first few days, maintain gentle oral hygiene, and attend your follow-up appointment to confirm healing is progressing well.